Articles
Calcium and Osteoporosis
Osteoporosis is the abnormal loss of calcium from the bones, which causes them to weaken and become more susceptible to fractures.
The Calcium Story
Calcium is essential throughout life. 99% of the body's calcium is stored in the bones and teeth. 1% calcium is distributed in the body fluids and soft tissues.
Blood calcium is kept constant by a balance of calcium between the bones and the blood. If calcium is not available from food, the storehouse in the bones will gradually be depleted.
Our bones reach their peak bone mass by the age of 20 to 25 years with the greatest increase in mass during adolescence. Even after peak bone mass has been attained we still need calcium to maintain strong bones.
The point at which they reach their peak strength is called peak bone mass.
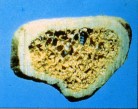 |
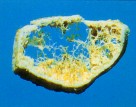 |
| Normal bone Peak bone mass |
Osteoporotic bone Low bone mass |
The potential for osteoporosis depends on both the peak bone mass and the rate at which bone is lost.
At about 35 years, bones slowly start to lose calcium. Men lose up to 1% per year over the age 35 and so do women, except around menopause, when the rate for women accelerates considerably.
This is due to a decrease in oestrogen (female hormone), which plays a central part in maintaining bone balance in women.
Bone loss during menopause appears to be the major reason that women are at a greater risk of osteoporosis than men.
The danger level where bones break more easily because of their reduced bone mass is called the fracture threshold which occurs at around the mid to late sixties for women, and the late eighties for men.
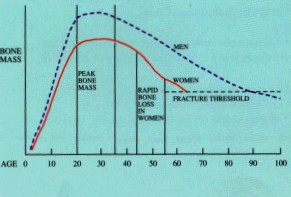
The more calcium you have stored in your bones, the less likely you are to get osteoporosis and fractures.
Bone is a living, growing structure and like muscle, putting bones under stress or 'making them work", stimulates their development. The simplest way to make them work is weight bearing exercise eg walking. It is important that we participate in at least 30 minutes of weight bearing exercise on most days of the week.
The National Health and Medical Research Council of Australia recommends the following daily intake of calcium
The best source of dietary calcium is dairy foods eg milk, cheese, and yoghurt. Aim for 3 serves of dairy foods daily or 3 serves of calcium fortified soy products. If fat or cholesterol is a problem, choose low fat dairy products. Smaller sources of calcium are obtained from canned fish with bones, grains, vegetables, nuts and seeds. If it is difficult for you to obtain adequate calcium from your diet, you need to consider a calcium supplement. Calcium supplements are best taken before bed because calcium uptake by bones peaks during the night. Excess calcium can accumulate in the kidneys causing kidney stones. Check with your doctor before taking calcium supplements, especially if there is a family history of kidney stones. There is now available a Bone Mineral Density (BMD) test which accurately predicts the chances of developing osteoporosis. The BMD measures the concentration of minerals in bones to determine how strong and resistant to fractures they are. It is advisable to have a BMD at the start of menopause before the damage is done. If treatment is begun at the time of menopause calcium loss from bones can be minimised. Once humping of the spine or fractures have occurred it is difficult to replace the calcium that has been leached out. The best treatment requires calcium supplementation and hormone replacement therapy (HRT), together with regular weight-bearing exercise eg walking and exercise using light-weights. HRT is the most effective method of preventing osteoporosis. It maintains bone size and strength and minimises fractures. HRT is usually a combination of oestrogen and progesterone and ideally therapy begins when oestrogen deficiency first appear early in menopause. Although there are some risk factors we cannot alter, there are things we can do to increase or maintain the strength of our bones to help protect ourselves against osteoporosis.
These habits should start in childhood and continue through out life.
Added to site on : Monday, 20 December 2010
�
Age
Calcium
Boys
8-11 years
1000
�
12-15 years
1300
�
16-18 years
1300
�
�
�
Girls
8-11 years
1000
�
12-15 years
1300
�
16-18 years
1300
�
�
�
Men
19-64 years
1000
�
66+ years
1300
�
�
�
Women
19-54 years
1000
�
54+ years
1300
Pregnant
Last 3 months
1000
Lactating
�
1000
FOOD SOURCES PROVIDING APPROXIMATELY 300 mg CALCIUM Quantity Food Kilojoules Calories 250 ml Whole Milk 700 167 215 ml Hilo Milk 510 122 200 ml Browne�s Non-fat Milk 315 75 175 ml Pura Tone 335 80 160 ml Calcium Plus or Fitness Milk 360 85 24 g
(3 level tabsp)Skim Milk Powder 360 85 250 ml So Good Soy Milk 650 155 200 g Yoghurt- Natural No-fat 500 120 200 g Yoghurt- Flavoured Non-fat 690 165 35 g Cheddar Cheese 580 140 38 g Devondale No 7 (7%fat) Cheese 220 52 360 g Creamed Cottage Cheese 1635 390 260 g Low fat Cottage Cheese 995 240 100 g Canned Sardines with bones 835 200 100 g Canned Salmon with bones 670 160 6 only Oranges 1758 420 1 kg Broccoli 980 230 20 slices Wholemeal Bread 2600 620 120 g Chocolate (20 squares) 2680 640 230 g Ice cream (over 4 large scoops) 1725 414 30 g Sesame seeds not hulled, they usually are 730 175 130 g Almonds 3080 735 Calcium Supplements
Test for Osteoporosis
Treatment
Risk Factors in Osteoporosis
In Summary - How can we prevent osteoporosis

